

Swallowing Disorders
Difficulty swallowing is a disturbing symptom that occurs in the vast majority of patients with a serious life-limiting illness. In fact, swallowing disorders, distinct from diminished appetite, are part of the natural process at the end of life, irrespective of the etiology. Difficulty swallowing can impact the quality of life of the patient as well as of caregivers, whose natural instinct to nurture and comfort with food is curtailed. Dysphagia is a poor prognostic sign in patients nearing the end of life, and for many patients with a life-limiting illness, the inability to swallow may represent a pivotal symptom that prompts the decision to consider end-of-life or hospice care.
Swallowing disorders occur frequently in patients with malignancies of the upper aero digestive tract and brain as well as with progressive degenerative neurologic disorders, including dementia. But they can occur as a result of the general debility that develops in patients with a variety of medical illnesses who are near the end of life.
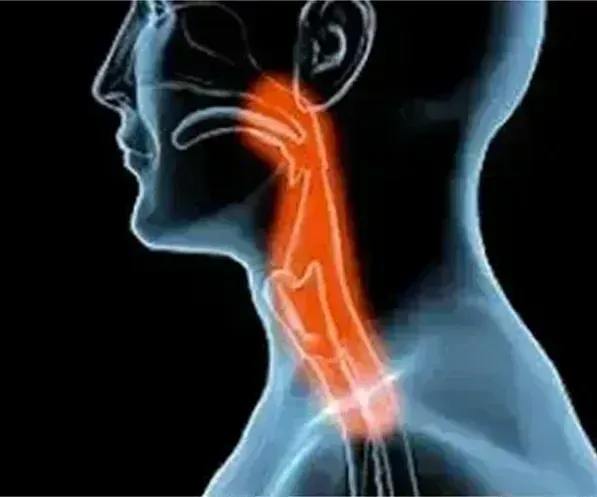
Detection of a swallowing disorder may elude the attention of both patients and caregivers. Silent aspiration (where food enters the upper airway without overt signs of coughing or choking) is a common correlate of dysphagia. In fact, 40 percent of patients who aspirate are said to aspirate silently, and this is more likely in individuals with a serious life-limiting illness where multiple causative factors coexist Clinicians should be alert for surrogate markers of dysphagia, such as general frailty, unexplained fever or cough with chills, alterations in secretion volume, color, or viscosity, chest pain, or dyspnea.