

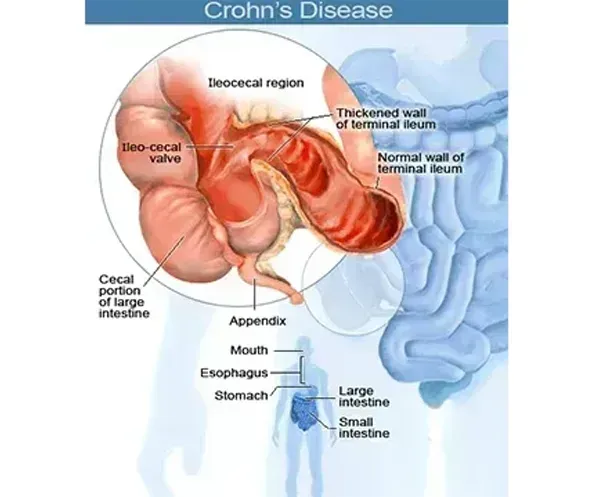
Crohn’s disease is an inflammatory condition that can affect any portion of the gastrointestinal tract from the mouth to the perianal area. Its transmural inflammatory nature coupled with the variability of intestinal distribution (i.e., which intestinal segment is affected) and systemic manifestations, gives rise to a spectrum of clinical presentations and long-term risks that have to be considered in deciding the optimal therapeutic approach.
The choice of therapy varies depending upon the anatomic location of disease, the severity of disease, and whether the treatment goal is to induce remission or maintain remission. Medical therapies that are used for Crohn disease include:
Crohn Disease Activity Index — Clinical trials of Crohn’s disease often use formal grading systems to describe disease activity. Two commonly used systems are the Crohn's Disease Activity Index (CDAI) (calculator 1) and the Harvey-Bradshaw Index (HBI) (calculator 2) [5], which is a simplified derivative of the CDAI. The HBI has been shown to correlate with the CDAI [6]. A drop in the CDAI of 100 points corresponds to a 3-point drop in the HBI. A CDAI of <150 (i.e., clinical remission) corresponds to an HBI of <4. These Crohn disease activity scoring systems rely on subjective symptoms, and while still utilized in clinical research trials, there is an emerging construct that defines disease burden in terms of objective findings and the presence or absence of bowel destruction. In addition, clinical trials are increasingly utilizing patient-reported outcomes to assess disease activity in Crohn disease.
Low- versus moderate/high-risk patients — In addition to the clinical parameters, the American Gastroenterological Association (AGA) stratifies patients into either a low or moderate/high risk category by assessing inflammatory status with the following tests:
Patients with mild Crohn disease who are at low-risk for long term sequelae usually have no or mild symptoms as described above and lack signs of systemic inflammation (i.e., normal or mild elevation in C-reactive protein and/or fecal calprotectin levels) (see "Clinical manifestations, diagnosis, and prognosis of Crohn disease in adults").
Patients initially identified as low risk may be subsequently reclassified as higher risk if they develop complications or don’t respond to initial treatment. Other prognostic factors associated with a more complicated disease course include bowel damage as measured by cross sectional imaging, extra-intestinal manifestations of disease, number of flares, need for glucocorticoids, and resultant hospitalizations.